 QUESTIONS D'ÉCONOMIE DE LA SANTÉ 2007
QUESTIONS D'ÉCONOMIE DE LA SANTÉ 2007
Issues in Health Economics
Issues in Health Economics (in French : Questions d'économie de la santé) is a monthly publication presenting syntheses of latest Irdes research on health economics. Benefiting from a high public visibility, this publication is systematically translated in English.
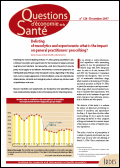
Delisting of mucolytics and expectorants: what is the impact on general practitioners' prescribing?
Questions d'économie de la santé n° 128. December 2007.
Devaux M., Grandfils N., Sermet C.
Following the round of delisting of March 1st, 2006, general practitioners' prescribing of mucolytics and expectorants for the treatment of upper and lower respiratory tract infections has reduced by a half. From this point of view the policy would appear to be effective. Nevertheless it seems that physicians are shifting their prescribing to other therapeutic classes, depending on the diagnosis, such as cough suppressants or bronchodilators, some non-steroidal antiinflammatories, corticoids and otological products, without any obvious medical justification in all cases.
Because mucolytics and expectorants are inexpensive, total prescribing costs have remained stable, despite a trend of increasing costs for other drug classes.
Medical group practice in primary care in six European countries, and the Canadian provinces of Ontario and Quebec: what are the lessons for France?
Questions d'économie de la santé n° 127. November 2007.
Bourgueil Y., Marek A., Mousquès J.
Medical group practice in primary care remains comparatively undeveloped in France compared to other countries. In Finland and Sweden, doctors are grouped in local public structures with multidisciplinary teams, whereas in Canada, the Netherlands and the United Kingdom, they are organised in private units run by independent health professionals on a contractual basis.
Among the factors explaining this trend, mention should in particular be made of a genuine political determination to place primary care at the heart of the health system and a definite change in health care supply and demand: increased demand for care in a context of decreasing medical density, need for improved health care coordination, the quest for less onerous working conditions and hours, etc.
This grouping often goes hand in hand with new rules and practices: voluntary registration procedures for patients with a doctor in group practice, greater cooperation between health professionals, changes in doctors' remuneration and new contracts between groups and health authorities. Certain signs are already visible in France, doubtless presaging an acceleration in the trend towards medical group practice.
Complementary health cover changes at retirement time - Analysis of retirees' switching behaviour
Questions d'économie de la santé n° 126. October 2007.
Franc C., Perronnin M., Pierre A.
On retirement, many complementary health insurance contract holders change provider: this is indeed the case for 51% of compulsory group contract holders, 39% of voluntary group contract holders and 23% of individual contract holders.
The higher mobility rates observed among group contract holders – especially those with a compulsory contract – can be confirmed after controlling for other characteristics that may explain this greater mobility, in particular their health status. This reflects the impact of the increase in group contract premiums for recently retired people, an increase that is primarily due to the loss of both group pricing and the employer's contribution. Their greater mobility may also mean that cover designed for a group of employees does not meet retirees' health care needs.
Mobility also depends on the type of health insurance provider managing the contract before retirement: People covered by commercial insurance companies change more frequently than those with contracts managed by mutuelles or provident institutions.
Bad health strongly increases the risk of becoming unemployed or inactive
Questions d'économie de la santé n° 125. September 2007.
Jusot F., Khlat M., Rochereau T., Sermet C.
An active person has many more risks of becoming non-employed1 if he/she suffers from health problems. According to this study, the short term risk of becoming inactive, within four years, is multiplied by 4 for persons suffering from a long term disease and by 1.5 for persons suffering from an incapacitating disease. The risk of unemployment is two times greater for persons who consider themselves as having bad health with respect to those who declare themselves in good health.
While the health condition is only one of the factors involved in the choice of individuals to stop working or in the decision of the employers to make them redundant, it must be taken into account, independently of strictly professional criteria such as diploma or experience, for a better understanding of professional trajectories.
Introducing Gate Keeping in France: first assessment of the preferred doctor scheme reform
Questions d'économie de la santé n° 124. July 2007.
Dourgnon P., Guillaume S., Naiditch M., Ordonneau C.
The Health insurance reform that came into effect in January 2006 encourages a “coordinated treatment pathway” (“ parcours de soins coordonnés”) in which the “Preferred Doctor ” (Médecin Traitant) plays a central role: Chosen by the patient, he is supposed to carry out primary care and orients the patient towards specialist care.
After one year implementation, we draw up an initial assessment of the preferred doctor scheme, (cf. box below) based on data from the Health, Health Care and Insurance 2006 survey and from the national public sickness fund insurance (Cnam). According to the latter in mid-2006 eight out of ten French had declared a preferred doctor to the fund1. The Health, Health Care and Insurance 2006 survey shows that persons voluntarily opting not to enter the scheme represent only 5% as the remaining (14%) declared having had no need to consult since the reform implementation. The new scheme is considered to be mandatory by a vast majority. The preferred Doctor very often replaces the previous family doctor informal scheme. The new system appears to be neutral regarding patient satisfaction with respect to medical treatment. Regarding specialist's access, less than 4% declared having given up for reasons directly related to the reform (they considered the new procedure too expensive or to complex). However, the survey data does not make possible to determine whether the care given up was actually medically unnecessary.
What do we suffer from? Evaluation of declared diseases in France - Decennial Health Survey, Insee 2002-2003
Questions d'économie de la santé n° 123. June 2007.
Allonier C., Guillaume S., Sermet C.
In 2002-2003, according to the Decennial Health Survey (EDS), eight out of ten persons declared suffering from at least one health disorder on a given day. More than one out of two persons declare eyesight problems (myopia, presbyopia, hypermetropia) or mouth and teeth diseases (caries, dental prosthesis). The most frequent diseases are then osteoarticular diseases, endocrine diseases, nutritional and metabolic diseases and cardiovascular diseases that affect approximately one out five persons.
The nature of the diseases evolves with age in particular, from the age of 40, with the appearance followed by the predominance of cardiovascular risk factors and diseases. Women declare more health problems than men and suffer more from depressive conditions, thyroid and venous insufficiency problems, while men declare more heart disease. Finally, variations are observed depending on the social situation: high blood pressure, diabetes and obesity are pathologies seen more frequently in persons with a disadvantaged social situation.
Improving the geographical distribution of practitioners: the measures adopted in France
Questions d'économie de la santé n° 122. May 2007.
Bourgueil Y., Mousquès J. , Marek A., Tajahmadi A.
Despite the fact that the density of medical practitioners has never been as high, the geographical and disciplinary distribution remains very unequal across France. This situation is likely to worsen given the decrease in the number of doctors that is predicted for the coming ten years.
For many years, an increase in the number of trained doctors and the regional adjustment of the numerus clausus and junior doctors' positions were the only measures taken to try and redress these imbalances.
More recently, new measurements aimed at encouraging doctors to set up practices in more difficult areas, be they rural or urban, have been implemented. On a national scale, the government and the Social Security service provide financial assistance for setting up or maintaining practices in these areas, as well as guidance and information. At a more regional level, the measures taken focus principally on training and provide support to initiatives undertaken by healthcare professionals who wish to organise their practices differently (group practices, task delegation, remote medicine).
Although few of these measures have so far been properly appraised, a number of results can nevertheless be underlined. These results can be set against the findings from international literature on the subject.
Helping the poor to acquire a complementary health insurance: an initial appraisal of the ACS system
Questions d'économie de la santé n° 121. April 2007.
Franc C., Perronnin M.
This study is an appraisal of the complementary health insurance acquisition assistance system called Aide complémentaire santé (ACS), first set up in January 2005. The objective of this financial aid is to help people who have an income just below the threshold enabling them to benefit from universal complementary health coverage (CMU-C) to obtain complementary health insurance coverage.
Despite a regular increase in uptake, one year after being set up the system concerned only a little over 200,000 people. This result was far below the 2 million people initially targeted by the measure and announced by the government when it was implemented. The analysis of the contents and price of the complementary health insurance contracts demonstrates that subscribing households, even after having benefited from the ACS, are still contributing considerable sums with respect to their total income. The system currently leaves beneficiaries paying almost 60% of the price of the contract, i.e. an average of €389 a year, which represents around 4.5% of their annual income. This is an overhead which is much higher than that borne on average by other insured households, despite the fact that they choose cheaper contracts which therefore offer average or even poor levels of reimbursement for traditionally poorly refunded care such as eye and dental treatment.
Hospital at home, an economical alternative for rehabilitative care
Questions d'économie de la santé n° 119. February 2007.
Afrite A., Com-Ruelle L., Or Z., Renaud T.
The need for dedicated beds for rehabilitative care (RC) shall increase over the coming years, in particular for the elderly. This type of care, dispensed mainly by inpatient hospital structures, is also being developed recently in the context of at-home hospitalization (AHH). In the current political context, which is favourable to the creation of new AHH places, our study compares the costs of these two overlapping healthcare methods. We estimate that half of the care provided as inpatient rehabilitation can be performed in AHH.
For those types of care that we consider «comparable» the average dailly cost, for public funding bodies , is €263 for inpatient RC compared to €169 for AHH. The difference goes down for elderly and/or highly dependent patients, but the daily cost for inpatient RC remains higher, whatever the patient's age, level of dependency and medical profile.
In order to face the needs of an ageing population, the creation of, for example 10,000 AHH places would represent, in the long-term, a saving of nearly 350 million euros per year for public funding bodies. AHH therefore represents an interesting economic alternative. It cannot, however, be considered for all patients as it virtually always requires the presence of a supportive entourage.
Inequality of opportunities in health: the influence of parents' social status and health status
Questions d'économie de la santé n° 118. February 2007.
Devaux M., Jusot F., Trannoy A., Tubeuf S.
We may consider the role of social and familial determinism among the range of causes of inequality of opportunity in health. Health status in adulthood is affected by an individual's social background. Two hypotheses are proposed in the literature: the direct effect of living conditions during childhood on adult health; the indirect effect of the family background on the future socio-economic status. We propose a third hypothesis in our study: the health status transmission from one generation to the next, based on a common genetic inheritance, and copying parental behaviours (health preferences, risky behaviours).
These three hypotheses are tested for the first time on French data from the 2004-2005 SHARE survey. The results suggest that health status in adulthood is directly affected by the mother's social status, and that father's social status has an indirect effect given its influence on childhood socioeconomic status. Without disregarding the effect of social background, the health status of both parents has a direct effect on the descendant's health in adulthood. Finally, the role of education is of importance as education level has a significant effect on social inequalities in health in adulthood.
